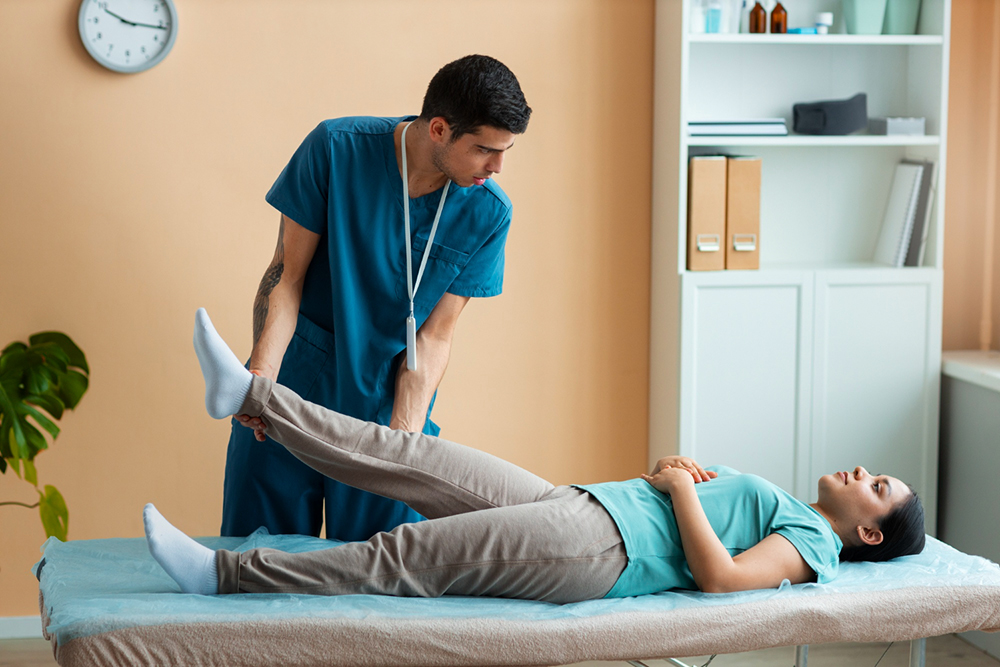
Do You Use Health Insurance for Physical Therapy?
If you've recently been injured or are recovering from surgery, your doctor may recommend physical therapy. While it's a key step in many recovery journeys, a question many people ask is: do you use health insurance for physical therapy? The short answer is yes, most health plans do offer some level of coverage, but the details vary. Knowing what your insurance covers and how to navigate the system can make a big difference in accessing the care you need without facing unexpected costs.
Let's explore how physical therapy and health insurance intersect and what you need to know to make the most of your benefits.
Is Physical Therapy Covered as Part of My Plan?
Most health insurance plans, including those under the Affordable Care Act (ACA), cover physical therapy if it is considered medically necessary. This typically means a doctor or specialist must prescribe physical therapy to treat an illness, injury, or chronic condition. Employer-sponsored plans, Medicare, Medicaid, and individual ACA marketplace plans generally include some type of coverage for rehabilitative services. However, the extent, such as the number of sessions covered or the types of therapies that qualify, depends on your plan.
What Is Physical Therapy?
Physical therapy (PT) is a form of treatment designed to enhance movement, alleviate pain, and restore function. It's typically used after surgeries, injuries, or as part of treatment for chronic conditions like arthritis or neurological disorders. Therapists use a variety of techniques, including advised exercises, stretches, manual therapy, and even specialized equipment, to aid patients in recovering their mobility and resilience.
Types of Insurance Coverage for Physical Therapy
There are several forms of insurance that may cover physical therapy:
- Private Health Insurance (including employer-sponsored and ACA plans): Usually covers PT as an essential health benefit.
- Medicare: Part B typically covers 80% of outpatient PT after you meet the deductible.
- Medicaid: States may offer PT coverage, but benefits can vary.
- Veterans Affairs (VA) & TRICARE: Offer PT benefits for eligible members.
- Auto Insurance (in case of accidents): Some policies include MedPay or Personal Injury Protection (PIP), which may cover PT.
Whether it's for accident recovery or managing a chronic condition, do you use health insurance for physical therapy? If you have any of the above coverage types, you likely can, but it's crucial to understand how your specific plan applies
Questions to Ask Your Physical Therapist
Before you start therapy, have a clear conversation with your provider. Ask:
- Do you accept my insurance plan?
- Are you in-network?
- Will I need a referral or pre-authorization?
- What out-of-pocket costs should I expect?
- How many sessions are typically covered?
These questions can help you avoid billing surprises and ensure your therapy stays within your insurance benefits.
Can My Health Insurance Deny Coverage for a Car Accident?
Yes, it's possible, though uncommon, for your health insurance to deny coverage for injuries from a car accident. This usually happens due to specific policy exclusions. For instance, some older or less comprehensive plans may state that health insurance won't cover car accident injuries, especially if auto insurance should be the primary payer. In other cases, coverage may be denied if the treatment isn't deemed medically necessary or if there's missing documentation or pre-authorization. It's important to understand the terms of your policy and know what's required to get your claims approved. If you're in an accident, be sure to document everything thoroughly and check whether your auto insurance coverage (like PIP or MedPay) applies first. If you're ever in doubt or confused, contact your insurance provider directly. This helps avoid unexpected surprises where health insurance won't cover car accident expenses you assumed were included.
How to Verify Physical Therapy Coverage
Not sure what your plan covers? Here's how to find out:
- Check your insurance provider's website: Look for documents labeled "Summary of Benefits and Coverage (SBC)."
- Call the customer service number on your insurance card: Ask about deductibles, copays, coverage limits, and pre-authorization requirements.
- 3. Ask your primary care provider or therapist's office: They often have staff who handle insurance verification and can help clarify your benefits.
This step is critical, especially if you're planning multiple sessions. Coverage limits or missing prior charges can result in denied claims.
The Role of Physical Therapy Clinics in Insurance Matters
Many physical therapy clinics are well-versed in insurance handling. Larger clinics often have billing coordinators who:
- Confirm your insurance benefits
- Submit paperwork for pre-authorization
- Track your remaining covered sessions
- Help appeal denied claims
This administrative support is invaluable when you're focused on healing. Some clinics may also offer guidance on switching to a different insurance-friendly provider if needed.
Does Insurance Cover Physical Therapy in Every Case?
No, not always. Insurance typically only covers PT that's medically necessary and part of a treatment plan. It won't cover therapy for general wellness, fitness goals, or maintenance therapy (unless tied to a medical condition). Insurers also often cap the number of sessions per year or require periodic evaluations to continue coverage.
If you're going for post-surgery rehab, you'll likely get approval quickly. However, if you're seeking PT for long-term pain or preventative care, you might face more scrutiny from your insurance provider.
Do Physical Therapists Take Insurance Even When They Are Not Part of Any Network?
Some therapists are out-of-network but still accept insurance. In these cases, they may:
- Ask you to pay upfront and submit a claim for reimbursement
- Submit a claim on your behalf (but at out-of-network rates)
- Charge higher fees compared to in-network providers
To avoid unnecessary expenses, it's always better to stick with in-network therapists unless you're willing to pay extra for a specific specialist.
How to Find Physical Therapists Covered by Insurance
To find covered providers:
- Use your insurance company's online directory
- Ask your doctor for referrals to in-network therapists.
- Call clinics directly and ask if they accept your insurance.
- If you have an ACA plan, visit healthcare.gov and log in to your plan to find in-network care options.
Finding a provider that fits both your medical and financial needs is the key to a stress-free recovery.
What to Do If You Can't Afford Physical Therapy
Not everyone has insurance, and even those who do may struggle with high deductibles or limited session coverage. If you can't afford PT:
- Ask about payment plans or cash discounts at your clinic.
- Look for community health centers that offer low-cost rehab services.
- Contact local universities with physical therapy programs — some offer supervised sessions at reduced costs.
- Check eligibility for Medicaid or other state-funded programs.
Don't let cost prevent you from recovering fully. Talk openly with your provider about your financial situation; many are willing to help.
Final Thoughts
So, do you use health insurance for physical therapy? In many cases, you can and should leverage your health insurance to make this vital care more affordable. Physical therapy can be a life-changing part of your recovery, and learning how to navigate insurance coverage can help you get the care you need without added stress.
By asking the right questions, verifying your coverage early, and staying in-network when possible, you can take full advantage of your health benefits and focus on what matters most: getting better.
Disclaimer: The information provided on this blog is for informational purposes only and is not intended as medical advice. Always consult with a qualified healthcare professional before making any health-related decisions.
Source: healthcare.gov

